Introduction
Irritable bowel syndrome treatment starts with understanding that the condition is not “just in your head”it’s a real, physical disorder that affects the way your gut and brain communicate. As a licensed therapist and medical educator, I’ve seen countless patients struggle with IBS symptoms that disrupt their work, social lives, and peace of mind.
The good news? IBS is manageable. With the right approach, most patients can reduce their symptoms and regain control of their daily lives. Unfortunately, many people unknowingly make mistakes that make their condition worse often due to misinformation online or self experimentation without proper guidance.
In this article, I’ll explain the 7 most common mistakes people make in irritable bowel syndrome treatment, what the latest science says, and how you can create a realistic, long term management plan that works.
What is the best treatment of Irritable Bowel Syndrome?
The best treatment of IBS depends on the type of IBS (constipation predominant, diarrhea predominant, or mixed). Irritable bowel syndrome treatment usually includes lifestyle changes, dietary changes such as a low FODMAP plan, stress management, and symptom targeted medications. For constipation, soluble fiber such as psyllium and mild laxatives may help. For diarrhea, loperamide or rifaximin may be prescribed.
Mental health support, including cognitive behavioral therapy (CBT), is often effective because IBS involves gut brain communication. Probiotics and gradual exercise can also reduce bloating and abdominal pain. Most patients improve when treatment is appropriate and consistent.
Understanding the nature of IBS
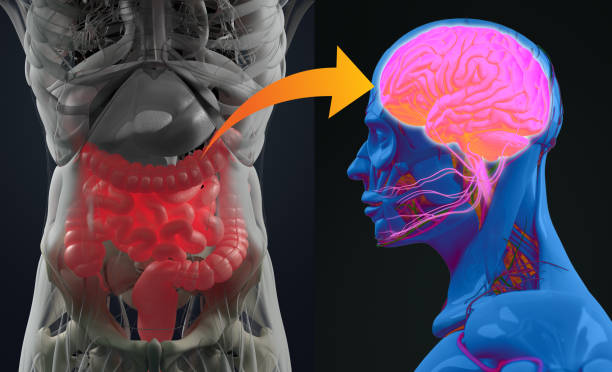
IBS is a gut brain interaction disorder.
IBS is classified as a disorder of gut brain interaction (DGBI). This means that the nerves that control your digestive system become overly sensitive, sending exaggerated signals to your brain. This can cause abdominal pain even when tests show your intestines to be completely normal.
A landmark study in Gastroenterology (2021) found that more than 70% of IBS patients have altered gut brain signaling, proving that it’s not psychological it’s physical.
Common Symptoms
- Abdominal pain or cramping
- Bloating and gas
- Constipation, diarrhea, or alternating between the two
- A feeling of incomplete bowel movement
These symptoms can also flare up during stressful periods, after certain meals, or due to hormonal changes.
Read more: Symptoms of Irritable Bowel Syndrome
7 Common Mistakes That Make IBS Symptoms Worse
1. Ignoring personal dietary triggers
Many people start a restrictive diet without professional help, hoping to “cure” their IBS. This often backfires. Each person’s gut sensitivities are unique what triggers one patient may be harmless to another.
Example:
A young woman I treated avoided all dairy for months, assuming it was the culprit. Her symptoms did not improve because the real problem was too much onion and garlic (high FODMAP foods).

What to do instead:
- Work with a dietitian for a short term low FODMAP trial (2-6 weeks).
- Reintroduce foods slowly to identify triggers.
- Don’t eliminate entire food groups without reason.
Read more: Best foods for irritable bowel syndrome
2. Overusing fiber supplements or using the wrong kind
Fiber is often recommended for IBS, but not all fibers are created equal. Soluble fiber (like psyllium husk) helps soften stools and support gut bacteria, while insoluble fiber (like wheat bran) can worsen bloating and pain in sensitive patients.
Medical insight:
A 2019 American Journal of Gastroenterology review found that soluble fiber improved IBS symptoms in 54% of patients, while insoluble fiber worsened them in about 30%.
What to do instead:
- Increase psyllium gradually for constipation.
- For diarrhea, use fiber sparingly and focus on hydration.
- Avoid sudden high fiber diets increase slowly.
3. Relying on medication alone
Many people expect a pill to “fix” IBS. Unfortunately, IBS does not respond to one size fits all medications. Medications are helpful, but only when paired with diet, stress management, and lifestyle changes.
Common Medical Treatment of IBS include:
- Loperamide for diarrhea
- Osmotic laxatives or linaclotide for constipation
- Antispasmodics for abdominal pain
- Low dose antidepressants (TCAs or SSRIs) for nerve related gut pain
Doctor’s insight:
I often explain to patients that IBS is like a sound system with multiple volume knobs. Medication adjusts one knob but diet, sleep, and stress control the others. You need to balance them all for relief.
4. Underestimating Stress and the Gut Brain Connection
Stress doesn’t cause IBS, but it does aggravate it. The gut and brain are connected by the vagus nerve, which controls digestion. When you’re anxious, the brain releases stress hormones that slow or speed up bowel movements, resulting in flare ups.
Scientific fact:
The Mayo Clinic notes that mind body therapies like CBT and mindfulness can significantly reduce the severity of IBS symptoms.
Simple strategy:
- Breathe deeply for 10 minutes daily.
- Light exercise like yoga or walking
- Journaling or guided meditation apps
Read more: Irritable Bowel Syndrome Explained
5. Not recognizing IBS subtypes
A key step in treating irritable bowel syndrome is identifying your subtype:
- IBS-C: Constipation predominant
- IBS-D: Diarrhea predominant
- IBS-M: Mixed pattern
Everyone requires different management. For example, a patient with IBS-D should not use the same high fiber plan as a patient with IBS-C.
Doctor’s advice:
I have had patients frustrated with “failed treatments” because their regimen targeted the wrong subtype. Recognizing your IBS pattern helps personalize therapy and avoid wasted effort.
Read more: Diagnosing irritable bowel syndrome
6. Neglecting the health of your gut microbiome
The gut microbiome the trillions of bacteria inside your intestines plays a key role in digestion, immunity, and inflammation. In IBS, studies often show an imbalance (dysbiosis) of these bacteria, often following infection or antibiotic use.
Unique insight:
While probiotics are helpful, not all are created equal. Many over-the-counter brands are unregulated and ineffective. A PubMed review (2020) concluded that Bifidobacterium infantis 35624 and Lactobacillus plantarum 299v are the most studied strains for IBS.
What to do:
- Try a 4-8 week course of probiotics containing these strains.
- Support microbiome health with a varied diet rich in fruits, vegetables, and fermented foods
7. Skipping Professional Follow up
IBS can be chronic, but that doesn’t mean you have to manage it indefinitely. Regular follow up ensures that your symptoms aren’t hiding something more serious, like inflammatory bowel disease, celiac disease, or colorectal cancer.
When to see your doctor:
- Unexplained weight loss
- Blood in the stool
- Persistent vomiting or severe pain
- Onset after age 50
Real world example:
One of my patients managed her IBS well for years but later developed anemia. Further testing revealed celiac disease. Regular follow up allowed for early detection.
Evidence based treatment of IBS that actually work.
Now that we’ve identified common mistakes, let’s discuss proven treatment of IBS so that sufferers achieve long term relief.
1. Lifestyle adjustments
- Eat slowly and chew well to reduce swallowed air.
- Avoid skipping meals; consistent timing helps with bowel rhythm.
- Stay hydrated aim to drink 6-8 glasses of water per day.
- Exercise for at least 150 minutes per week.
2. Dietary modifications
- Start with a supervised low FODMAP trial.
- Identify trigger foods (e.g. beans, onions, milk, wheat).
- Reintroduce foods one at a time.
- Avoid carbonated drinks and alcohol during flare ups.

3. Stress Management and Mind Body Therapies
There is a strong connection between the gut and the brain, often called the gut brain axis. For many IBS sufferers, stress, anxiety, or emotional distress can trigger or worsen symptoms. That’s why addressing mental health is just as important as treating the gut itself.
Cognitive Behavioral Therapy (CBT)
CBT helps patients identify and change thought patterns that cause anxiety and exacerbate bowel discomfort. Studies have shown that CBT can significantly reduce bloating, abdominal pain, and irregular bowel habits by improving the way your brain interprets bowel sensations.
Gut Directed Hypnotherapy
This is a specialized form of hypnosis that teaches relaxation and positive imagery focused on gut function. Research has shown up to 70% improvement in IBS symptoms after a Gut Directed Hypnotherapy session.
Yoga and Meditation
Gentle yoga stretches, deep breathing, and mindfulness meditation reduce stress hormones and improve digestion. Just 20-30 minutes a day can help regulate bowel movements and reduce abdominal discomfort.
As a doctor, I have seen patients experience significant improvements in IBS symptoms simply by incorporating mindfulness or yoga into their daily routine without changing any medications.
4. Medical Treatment of IBS
Sometimes, lifestyle changes and diet aren’t enough. When symptoms persist, medical treatment under the supervision of a healthcare provider may be necessary. medical treatment of IBS include:
Antispasmodics
These medications (such as hyoscine butylbromide or dicyclomine) help relax the muscles of the intestines, reducing cramps and pain. They are often prescribed for IBS with predominant pain or bloating.
Laxatives and fiber supplements
For IBS with constipation (IBS-C), osmotic laxatives such as polyethylene glycol (PEG) or soluble fiber supplements (such as psyllium) can soften stools and promote bowel regularity. Avoid stimulant laxatives unless recommended by a doctor.
Antidiarrheal agents
For IBS with diarrhea (IBS-D), medications such as loperamide slow down gut transit, reducing stool frequency. However, they do not treat the underlying sensitivity so they are often combined with other treatments.
Low dose antidepressants
Tricyclic antidepressants (TCAs) or selective serotonin reuptake inhibitors (SSRIs) are sometimes used in low doses not for depression, but to regulate gut brain communication. They reduce gut hypersensitivity and improve pain tolerance and used as treatment of IBS.
New targeted drugs
For severe or refractory cases, new agents are available as treatment of IBS:
- Lubiprostone or linaclotide for IBS-C
- Eluxadoline or rifaximin for IBS-D
These drugs target specific pathways in the gut to normalize bowel movements and reduce discomfort.
5. Probiotics and gut microbiome support
Your gut microbiome the trillions of bacteria inside your intestines plays a critical role in digestive and immune balance. In IBS, the composition of bacteria is often disrupted (dysbiosis).

Probiotic supplements as irritable bowel syndrome treatment
Probiotics are live “good bacteria” that restore balance in the gut. Strains such as Bifidobacterium infantis, Lactobacillus plantarum, and Saccharomyces boulardii have been shown to reduce bloating, gas, and discomfort.
Prebiotic Foods
Prebiotics (fibers that feed gut bacteria) include garlic, onions, asparagus, and oats. However, some IBS patients are sensitive to them due to their FODMAP content, so they should be introduced gradually.
Personalized Microbiome Therapy
Emerging research suggests that personalized microbiome analysis may aid in probiotic therapy. In the future, treatments may include bacteria custom designed to match an individual’s gut profile.
Tip: Keep a food and symptom diary to see how your body reacts to specific probiotic strains or prebiotic foods.
When to see a doctor.
Although IBS is a chronic condition, new or worsening symptoms should never be ignored. Seek immediate medical attention if you experience:
- Unintentional weight loss
- Bleeding from the rectum or black stools
- Persistent vomiting
- Severe abdominal pain that interferes with daily life
- A family history of colorectal cancer or celiac disease
Early diagnosis ensures that serious conditions such as inflammatory bowel disease (IBD) or colon cancer are not missed.
Conclusion: Living comfortably with IBS
Irritable bowel syndrome doesn’t have to control your life. With a thoughtful combination of dietary adjustments, stress management, and targeted medical care, most people can effectively manage IBS.
Remember every gut is unique. What works for one person may not work for another. So, work with your doctor to personalize your plan, and never stop listening to your body.
As a doctor, I tell my patients: Healing your gut is a journey, not a race. Be patient, be persistent, and celebrate every small victory.
Call to action:
If you found this guide helpful, explore more evidence based articles on LifeCareCure.com your trusted source for expert medical insights, gut health advice, and practical wellness tips.
References:
1. General Overview of IBS
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) IBS Overview
FAQS
Yes, most are safe but effectiveness depends on the strain. Discuss probiotic choices with your healthcare provider for the best match.
Absolutely. Stress and anxiety directly affect gut motility and sensitivity. That’s why relaxation therapies are a cornerstone of IBS treatment.
No, IBS currently has no permanent cure—but it can be effectively controlled. With the right diet, stress management, and lifestyle habits, many people experience long periods of symptom-free living.
Apply a warm compress to your abdomen, sip peppermint tea, avoid trigger foods, and practice slow breathing to relax your gut muscles.
🧑⚕️ About the Author
Dr. Asif, MBBS, MHPE
Dr. Asif is a licensed medical doctor and qualified medical educationist with a Master’s in Health Professions Education (MHPE) and 18 years of clinical experience. He specializes in gut health and mental wellness. Through his blogs, Dr. Asif shares evidence-based insights to empower readers with practical, trustworthy health information for a better, healthier life.
⚠️ Medical Disclaimer
This blog is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard or delay medical advice based on content you read here.


Leave a Reply