Introduction
What causes cirrhosis of the liver other than drinking is a question I hear often in my clinical practice. Many people associate cirrhosis with heavy alcohol use alone, but the truth is more complex. As a physician and medical educator, I want to guide you through the lesser known causes of cirrhosis, using simple explanations and real world examples and also will answer one important question that can Cirrhosis be prevented?
Think of your liver as the body’s central processing factory it clears toxins, manufactures proteins, and manages energy supplies. When the factory is repeatedly injured whether by infections, fat buildup, or toxins normal tissue is replaced with scar tissue. This scarring process is what we call cirrhosis. And just like an old machine running on rusty gears, a scarred liver can’t function efficiently.
What causes cirrhosis of the liver other than drinking?
What causes cirrhosis of the liver other than drinking is the concern of many individuals who are not drinker and often asked me this in my clinic ,Cirrhosis of the liver can be caused by many factors other than alcohol. The most common non alcoholic cirrhosis causes include chronic viral hepatitis (hepatitis B and C), non-alcoholic fatty liver disease (NAFLD), autoimmune hepatitis, inherited metabolic disorders such as hemochromatosis and Wilson’s disease, long-term exposure to toxins or certain medications, and long term illnesses. These conditions damage liver cells over time, resulting in scarring and decreased liver function. Early diagnosis and proper management are key to preventing the progression of cirrhosis.
1. Viral hepatitis – a silent global epidemic
Viral infections are among the top answers when we ask what causes non alcoholic liver cirrhosis. Hepatitis B and C viruses attack liver cells, triggering chronic inflammation.
- Hepatitis B affects approximately 296 million people worldwide (WHO, 2022).
- Hepatitis C remains the leading cause of cirrhosis and liver cancer.
Studies show that chronic viral hepatitis is one of the leading causes of non alcoholic cirrhosis worldwide. According to the World Health Organization (WHO), hepatitis B and C together are responsible for about 50% of cirrhosis cases worldwide. Research shows that 15-40% of people with chronic hepatitis B eventually develop serious liver complications, including cirrhosis and cancer. Similarly, 20-30% of patients with chronic hepatitis C progress to cirrhosis within 20-30 years if left untreated.
As a practicing physician, I often remind my patients that hepatitis can silently damage the liver for years without any obvious symptoms. This silent progression is why early diagnosis, antiviral treatment, and regular monitoring are absolutely essential to prevent cirrhosis.
Read in Detail About: [Causes of Hepatitis B] and [Symptoms of Hepatitis C in Men]
2. Non-alcoholic fatty liver disease (NAFLD) – Lifestyle-related damage
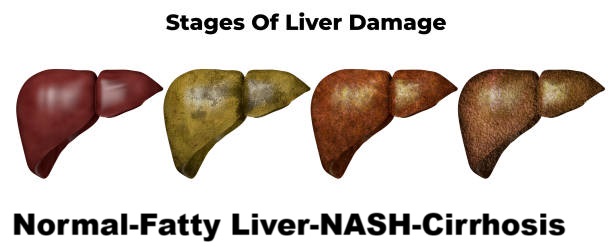
How fat builds up in the liver.
Imagine putting cooking oil in a sponge every day the sponge becomes heavy, greasy, and less efficient. That’s what fat does to the liver in NAFLD.
When fat builds up, it can progress to non-alcoholic steatohepatitis (NASH) an aggressive form that causes inflammation and finally progresses to non alcoholic cirrhosis.
Key risk factors:
- Obesity
- Type 2 diabetes
- High cholesterol
- Sedentary lifestyle
Read in Detail About: [Fatty liver disease]
3. Autoimmune hepatitis – When the body attacks itself.
In this rare condition, the immune system mistakes liver cells as “foreign invaders.” Over time, this friendly fire damages the liver, leading to cirrhosis.
Who is at risk?
- Women are more likely to be affected than men.
- It can occur with other autoimmune diseases, such as thyroiditis or rheumatoid arthritis.
Doctor’s insight: I once treated a young woman who came in with fatigue and joint pain. Blood tests revealed autoimmune hepatitis a reminder that cirrhosis is not always linked to lifestyle choices.
4. Genetic and metabolic disorders
Some people inherit medical conditions that silently damage their liver for many years. These disorders can remain hidden until cirrhosis has already developed. Early recognition allows for treatment that can prevent irreversible liver damage.
Hemochromatosis – Iron Overload
Hemochromatosis is one of the most common inherited liver disorders, affecting 1 in 200-300 people of Northern European descent (PubMed, 2020). The body absorbs too much iron, and the excess is stored in the liver, heart, and pancreas. Over time, this “iron rust” stains the liver and can also lead to diabetes and heart failure.
Doctor’s Insight: In my practice, I once diagnosed a man in his 40s with cirrhosis after unexplained fatigue and joint pain. His iron studies confirmed hemochromatosis. After treatment with regular blood draws (phlebotomy), his symptoms improved, showing how early intervention can save lives.
Wilson’s disease – copper buildup
Wilson’s disease is rare, affecting 1 in 30,000 people worldwide (WHO). It causes copper to build up in the liver, brain, and eyes. Patients may develop cirrhosis of the eyes, mood swings, or the classic “Kaiser-Fleischer rings.” Without treatment, it can be fatal in young adults.
Doctor’s insight: I once saw a young man refer to behavioral changes that were thought to be psychological. Further evaluation revealed Wilson’s disease, and chelation therapy (medications that remove copper) turned his life around. It’s a reminder that not all cirrhosis is lifestyle-related.
Alpha-1 Antitrypsin Deficiency – A protein defect.
This genetic defect affects 1 in 2,500 people of European descent (American Lung Association, 2022). The abnormal alpha-1 antitrypsin protein builds up in the liver, leading to chronic injury and cirrhosis. It also damages the lungs, resulting in early-onset emphysema, especially in smokers.
Doctor’s insight: The dual effect on both the lungs and liver often confuses patients. I describe it as “attacking two doors of the same house” if you treat only one, the other may fall. Therefore, both pulmonary and hepatic care are essential.
Glycogen Storage Diseases – Sugar Mismanagement
Glycogen storage diseases are rare, estimated to occur in 1 in 20,000-25,000 births (NIH). These disorders prevent the liver from storing or excreting sugar properly, putting stress on liver cells. In severe cases, children can develop liver enlargement, hypoglycemia, and cirrhosis before adulthood.
Doctor’s insight: I recall consulting a family whose child had recurrent low blood sugar and an enlarged liver. Genetic testing confirmed glycogen storage disease. Early nutritional management helped slow liver damage, showing how awareness can change long-term outcomes.
5. Long-term drug and toxin exposure
Some drugs, when used for years, can damage the liver. Examples:
- Methotrexate (used for joint pain and cancer)
- Amiodarone (for heart rhythm problems)
- High doses of vitamin A
- Environmental toxins such as aflatoxin (mold-contaminated grains) have also been linked to cirrhosis and liver cancer.
Reference: CDC – Toxins and Liver Disease
6. Bile duct diseases – hidden blockages.
When bile (digestive fluid) can’t flow properly, it irritates the liver and causes scarring.
- Primary biliary cholangitis (PBC) – spontaneous destruction of the bile ducts
- Primary sclerosing cholangitis (PSC) – chronic inflammation that causes hardening.
Patients may initially feel itchy and tired before liver damage becomes apparent.
7. The Chronic Heart Failure and Cirrhosis Connection
Few people realize that long-term heart failure can cause blood flow to the liver to back up, leading to “cardiac cirrhosis.”
This is a rarely mentioned but important cause of cirrhosis outside of alcoholism.
8. Infections and parasitic diseases
When people ask, what causes liver non alcoholic cirrhosis, infections are often overlooked. Yet, in many parts of the world, especially in developing regions, chronic infections and parasites are major culprits of non alcoholic cirrhosis. These conditions cause gradual liver damage, often without obvious early warning signs.
Schistosomiasis – a leading cause in tropical regions
Schistosomiasis, caused by parasitic worms, is one of the most important infectious causes of cirrhosis globally. According to the World Health Organization (WHO, 2023), more than 240 million people are affected worldwide, mainly in Africa, South America and parts of Asia. The parasites lodge in the blood vessels of the liver, triggering inflammation and fibrosis that eventually leads to non alcoholic cirrhosis.
Doctor’s insight: During my training, I saw patients in rural areas who had an enlarged spleen due to cirrhosis related to schistosomiasis and abdominal swelling. Unlike alcoholic cirrhosis, these patients had no history of alcohol abuse reminding us that environment and exposure play a huge role.
Chronic bacterial and viral infections
Recurrent bacterial infections of the liver, such as chronic liver abscesses, can cause scarring over time. In some cases, viruses other than hepatitis (such as cytomegalovirus in immunocompromised patients) can also contribute to long-term damage. Although less common, these infections act as repeated “attacks” on liver tissue, leaving scars behind.
Parasitic cysts and infections
Conditions such as echinococcosis (hydatid cyst disease) caused by tapeworm larvae cause cysts to form in the liver. If left untreated, these cysts rupture or become chronically inflamed, leading to fibrosis and non alcoholic cirrhosis in the long term.
Doctor’s insight: I once consulted a patient with a liver cyst that was initially suspected to be a tumor. Further imaging revealed a hydatid cyst, which was surgically removed. This case highlighted how parasitic infections can mimic other liver diseases and silently progress to cirrhosis.
Regional variations matter
Unlike Western countries where fatty liver and alcoholism are prevalent, infections and parasites remain the leading causes of cirrhosis in many tropical and subtropical regions. This highlights the importance of local epidemiology when evaluating a patient with liver disease.
Reference: WHO – Schistosomiasis Fact Sheet
9. Malnutrition and severe protein deficiency
In some regions, especially where poverty and food insecurity are widespread, long-term malnutrition becomes a hidden cause of non alcoholic cirrhosis. The liver relies on protein to repair damaged cells and maintain its structure. When protein intake is chronically low, the liver begins to shrink, stop working, and over time, become scarred. This is especially seen in children with severe malnutrition (such as kwashiorkor), but it can also affect adults with chronic illnesses or poor nutrition. Early nutritional support is crucial to prevent irreversible liver damage.
10. Cryptogenic Cirrhosis – The Mystery Cases
Despite modern medications, some patients develop cirrhosis for no apparent reason. Many of these “mystery” cases are later linked to undiagnosed NAFLD or autoimmune hepatitis.
Symptoms of Non Alcoholic Cirrhosis
- Fatigue
- Easy bruising
- Yellowing of the skin (jaundice)
- Swelling in the legs or abdomen
- Confusion (hepatic encephalopathy)
Can cirrhosis be prevented?
Many people ask, can cirrhosis be prevented? The answer is yes, in most cases it can be slowed, delayed, or completely avoided with the right measures. Here are practical steps:
Get vaccinated against hepatitis B.
Since viral hepatitis is a leading global cause, vaccination is the strongest answer. Can cirrhosis be prevented? It protects the liver from long-term damage.Read in Detail About:[hepatitis B vaccine adult schedule]
Early screening for hepatitis C
Modern treatments can cure hepatitis C in more than 95% of cases (CDC, 2024). This makes early detection important further evidence that cirrhosis is preventable.
Maintain a healthy weight
Obesity and fatty liver disease are on the rise worldwide. By keeping your weight in a healthy range through diet and exercise, you reduce your risk of scarring and show that cirrhosis can be prevented through lifestyle changes.
Limit your alcohol intake.
While we’re focusing on the reasons not to drink, minimizing alcohol consumption further reduces the strain on the liver. For many patients, doctors assure them that cirrhosis can be prevented by combining medical treatment with diet.
Use medications wisely.
Avoid overuse of painkillers, herbal supplements, or medications that can damage the liver. Always consult your doctor before long-term use. Safer Prescription Methods answers the question: Can medications prevent cirrhosis?Yes, if monitored.
Eat a balanced, protein-rich diet.
Malnutrition and protein deficiencies impair liver repair. Proper nutrition is a simple but powerful way to show that good food choices can prevent cirrhosis. Read in Detail About: [How to Keep Your Liver Healthy]
Regular check-ups for genetic conditions
For people with a family history of Wilson’s disease, hemochromatosis, or alpha-1 antitrypsin deficiency, routine testing ensures early diagnosis and treatment. This once again highlights that cirrhosis is preventable in high-risk families.
Avoid environmental toxins.
Avoiding exposure to aflatoxins (contaminated grains), industrial chemicals, and unsafe herbal products reduces the risk of liver scarring. Preventing exposure is another way to prove that cirrhosis can be prevented with awareness.
Conclusion and Call to Action
Cirrhosis is not just about alcohol. There are many hidden causes from viral hepatitis to fatty liver disease, autoimmune conditions, and even genetic disorders. As a doctor, I encourage you to take your liver health seriously, get screened, and seek medical advice early.
Have questions about your liver health? Leave them in the comments, share your story, or consult your doctor today.
FAQS
Early-stage liver damage may be reversible with treatment and lifestyle changes. But advanced cirrhosis is usually permanent. The goal is to halt progression and manage complications.
It varies. Some conditions like Wilson’s disease can cause cirrhosis within a few years, while others like fatty liver may take decades. Genetics, lifestyle, and co-existing conditions also play a role.
No. Fatty liver is an early stage where fat builds up but the structure is intact. Cirrhosis happens when scarring permanently damages liver tissue. However, untreated fatty liver can eventually progress to cirrhosis.
Young adults may develop cirrhosis from autoimmune hepatitis, Wilson’s disease, or chronic viral infections. These are often overlooked because cirrhosis is thought to be an “older person’s disease.” Early testing is crucial.
Globally, viral hepatitis (B and C) remains the leading cause of non-alcoholic cirrhosis. In developed countries, NAFLD is rapidly becoming the top cause due to rising obesity and diabetes.
🧑⚕️ About the Author
Dr. Asif, MBBS, MHPE
Dr. Asif is a licensed medical doctor and qualified medical educationist with a Master’s in Health Professions Education (MHPE) and 18 years of clinical experience. He specializes in gut health and mental wellness. Through his blogs, Dr. Asif shares evidence-based insights to empower readers with practical, trustworthy health information for a better, healthier life.
⚠️ Medical Disclaimer
This blog is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard or delay medical advice based on content you read here.



Leave a Reply