Introduction
Stage 4 cirrhosis of the liver life expectancy is one of the most frequently sought concerns by patients and families facing this advanced stage of liver disease. Understandably, the words “stage 4” and “cirrhosis” can seem overwhelming, often evoking fear and hopelessness. But as a licensed physician and medical educator, I want to assure you that despite the seriousness of the condition, there are many factors that affect how long a patient can live and importantly, there are practical steps that can make a positive difference.
In this article, I will explain stage 4 cirrhosis in simple, non-technical language, answer common concerns about life expectancy, and share ways for patients to live a long and strong life despite their diagnosis. I will also include unique clinical insights from real world practice, tips rarely discussed in competing blogs, and links to helpful resources like my guides on the Liver Cleanse Diet Plan and Cirrhosis Self Care
What is Stage 4 Cirrhosis of the Liver Life Expectancy?
Stage 4 cirrhosis is the most advanced stage of liver damage, where the liver has lost most of its ability to function. Life expectancy varies widely depending on the presence of complications, overall health, and access to treatment. On average, patients with stage 4 cirrhosis can survive from 6 months to several years. Those who do not have severe complications such as variceal bleeding, kidney failure, or liver cancer can sometimes live for more than 5 years with careful medical care and lifestyle changes. In contrast, those with recurrent complications may have a shorter life expectancy.
Importantly, medical advances, liver transplantation, and supportive care can significantly increase survival and improve quality of life. Each patient is unique meaning that a diagnosis should always be discussed with an expert rather than relying on general averages.
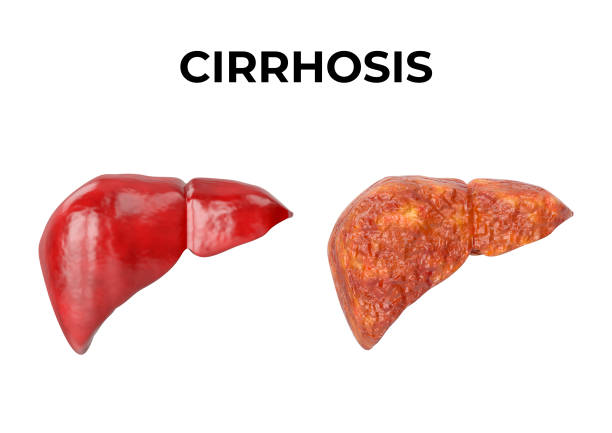
Understanding Stage 4 Cirrhosis
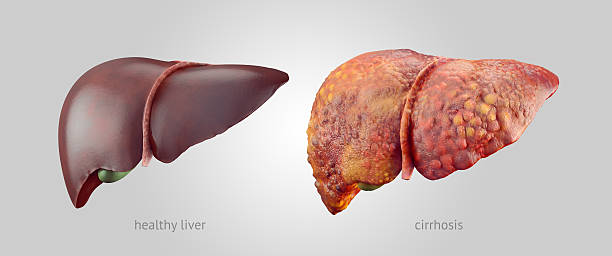
Stage 4 cirrhosis is often referred to as end stage liver disease. This does not mean that life is over. Instead, it means that the liver is severely scarred and struggling to function. Think of the liver as a sponge filter in the early stages, it can still filter blood despite some damage. By stage 4, most of the sponge has hardened, leaving only a small portion functioning.
What happens in stage 4?
- Extensive scarring (fibrosis) replaces normal liver cells.
- Blood flow through the liver is blocked, leading to portal hypertension.
- Complications such as fluid in the abdomen (swelling), bleeding, confusion (hepatic encephalopathy), and jaundice occur.
- The risk of liver cancer is significantly increased.
Stage 4 Cirrhosis of the Liver Life expectancy
Survival rate based on Child-Pugh classification.
Doctors often use the Child-Pugh score to estimate cirrhosis life expectancy:
- Class A (compensated): 15–20 years
- Class B (significant symptoms): 6–10 years
- Class C (created, stage 4): 1–3 years on average
(Source: PubMed, “Prognostic Indicators in Liver Cirrhosis,” PMID: 32442257)
MELD score and cirrhosis life expectancy
The Model for End-Stage Liver Disease (MELD) score predicts survival based on lab tests (bilirubin, INR, creatinine, sodium). A higher score means a shorter life expectancy.
- MELD 10–19 → Median survival 6+ years
- MELD 20–29 → 1–2 years
- MELD 30+ → Months without transplant
Factors that affect stage 4 cirrhosis of the liver life expectancy
Stage 4 Cirrhosis of the Liver life expectancy is not fixed it varies widely from person to person. Factors such as lifestyle choices, medical care, nutrition, and the presence of complications play a major role in shaping the outcome. Some patients survive for only months, while others, with the right support and treatment, can live for many years. Understanding what improves or worsens the prognosis helps patients and families take control where it matters most.
Factors that increase Cirrhosis life expectancy (protective)
Complete alcohol abstinence
Alcohol is one of the most destructive forces for a cirrhotic liver. Even small amounts can worsen scarring and accelerate complications. Patients who quit completely often stabilize, and in some cases, even mild improvements in liver function are seen.

Optimal nutrition and muscle preservation
Nutritional deficiencies and muscle wasting (sarcopenia) are silent killers in cirrhosis. A high-protein diet (unless restricted by your doctor), along with plenty of vegetables, fruits, and healthy fats, provides the liver with the building blocks it needs. Small, frequent meals especially snacks help prevent the body from breaking down its own muscle for energy.Read in detail About: [ How to Keep Your Liver Healthy] [ and [ Liver Cirrhosis Foods to Avoid ]
Tight control of complications
Regular medical monitoring can detect ascites, varices, or encephalopathy early. For example, scheduled endoscopy for varices can prevent life threatening bleeding, and diuretics along with salt restriction can effectively manage ascites.
Timely vaccinations and infection prevention
Infections in cirrhosis can quickly lead to liver failure. Vaccines against hepatitis A, hepatitis B, influenza, and pneumonia reduce the risk. Good hygiene, a safe diet, and early use of prescribed antibiotics also help.
Eligibility for a Liver Transplant
Screening for a liver transplant can change the prognosis. A successful transplant can extend life expectancy by decades, and even being “on the list” ensures close monitoring and priority care.
Strong emotional and social support
Patients with supportive families and active social lives tend to have better adherence to treatment and a stronger determination to fight. Stress reduction techniques such as meditation, light exercise, or spiritual practices also help stabilize health.
Consistent medical follow-up
Patients who see their hepatologist regularly, take prescribed medications, and have follow-up tests often live longer. Early detection of kidney changes, rising bilirubin, or occult blood allows for intervention before a crisis strikes.
Factors that shorten Cirrhosis life expectancy (risk)
Continued alcohol or drug use
Drinking after a diagnosis of cirrhosis is almost always fatal in the short term. Similarly, certain medications (non prescription painkillers, herbal supplements, or recreational drugs) can accelerate liver failure.
Uncontrolled viral hepatitis (B or C)
If hepatitis infection is left untreated, it continues to damage the liver. Patients who do not have access to antivirals deteriorate more rapidly than those who do.
Severe malnutrition and sarcopenia
Low body weight, vitamin deficiencies, and muscle loss weaken the immune system, increase the risk of infection, and reduce survival.
Recurrent or severe complications
- Ascites: Fluid in the abdomen that is difficult to control often indicates disease.
- Miscellaneous bleeding: Any major bleed reduces the chances of survival.
- Hepatic encephalopathy: Recurrent episodes indicate poor clearance of toxins by the liver.
- Hepatorenal syndrome: Kidney failure associated with cirrhosis is a serious diagnosis.
Liver cancer (hepatocellular carcinoma, HCC)
Cirrhosis is the strongest risk factor for HCC. Once cancer develops, survival depends on early detection and treatment options.
Poor adherence to medical care
Missing medications such as lactulose, skipping follow ups, or not adhering to dietary restrictions all increase complications.
Psychological stress and isolation
Depression and isolation worsen outcomes. Patients who lose motivation often neglect their own care, leading to avoidable deterioration.
Doctor’s note:
What really makes the difference in stage 4 cirrhosis of the liver life expectancy is the balance between controlling what you can (diet, alcohol, infections, follow up) and preparing for options such as transplant. People who actively engage with their health often live much longer than expected.
Unique insight of the doctor (rarely discussed)
In my clinical experience, an underestimated factor in the diagnosis of cirrhosis is the patient’s mindset and support system. Patients who are socially engaged, motivated, and emotionally supportive often cope much better than those who feel hopeless.
I recall a patient in his late 50s who was diagnosed with decompensated cirrhosis and given a 1 year survival estimate. With strong family support, lifestyle changes, and adherence to medical care, he lived 5 meaningful years, attended his daughter’s wedding, and even traveled. This rarely appears in the data, but it highlights the human dimension of healing.
Patient-friendly analogy
Imagine your liver as a city’s power plant. In stages 1-2, it’s like a minor malfunction in the machinery still working. By stage 4, most of the machines have shut down, and the backup generators are overloaded. However, with smart management, repairs, and even a new power plant (transplant), the city can still thrive.
Emotional and mental well-being
Stage 4 cirrhosis doesn’t just affect the body; it also affects emotions, family, and daily life.
- Find counseling or support groups
- Practice stress-reducing activities such as meditation or light walks.
- Stay socially connected; isolation has worse outcomes.

References:
World Health Organization – Liver Cirrhosis
Centers for Disease Control and Prevention (CDC) – Chronic Liver Disease
Conclusion and Call to Action
Stage 4 Cirrhosis Life Expectancy is a difficult topic, but numbers never tell the whole story. With modern medicine, liver transplantation, lifestyle changes, and emotional resilience, patients can live longer and more meaningful lives, according to the data.
As a doctor, I encourage you to focus not only on “how long” but also on “how well.” Every day can be made better with the right choices, care, and hope.
If you or a loved one is facing cirrhosis, check out my blogs on [ Cirrhosis Self-Care ]
and [ Liver Cleanse Diet Plan ] for practical guidance.
Your turn: Share your questions, concerns, or personal stories in the comments about cirrhosis life expectancy. I’d be happy to guide you further. If you need personalized advice, consult your liver specialist without delay.
FAQS
Yes. Avoiding alcohol, eating liver-friendly foods, reducing salt, and treating complications promptly can extend both life expectancy and quality of life.
Unfortunately, the scarring is permanent. However, progression can be slowed, and symptoms managed. Transplant remains the only curative option.
Yes. Patients with good emotional support, motivation, and stress management often cope better and live longer than those who feel isolated or hopeless.
For many patients, transplant offers the best long-term survival. However, supportive care, medications, and procedures can also improve outcomes significantly.
On average, it ranges between 1–3 years depending on complications. However, with proper care, some patients live beyond 5 years, especially if eligible for a transplant.
🧑⚕️ About the Author
Dr. Asif, MBBS, MHPE
Dr. Asif is a licensed medical doctor and qualified medical educationist with a Master’s in Health Professions Education (MHPE) and 18 years of clinical experience. He specializes in gut health and mental wellness. Through his blogs, Dr. Asif shares evidence-based insights to empower readers with practical, trustworthy health information for a better, healthier life.
⚠️ Medical Disclaimer
This blog is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard or delay medical advice based on content you read here.


Leave a Reply