Introduction
Hepatitis C in pregnancy is a health problem that often goes undiagnosed until complications arise. As a licensed physician and medical educator, I have seen how fear and confusion surround this diagnosis. Many expectant mothers ask me: “Will my baby be safe?” or “Can treatment wait until after delivery?”
The truth is that while hepatitis C can pose challenges during pregnancy, with the right knowledge and medical guidance, most women can still have a safe pregnancy and a healthy baby.
What is hepatitis C in pregnancy?
Hepatitis C in pregnancy refers to the presence of an active hepatitis C virus (HCV) infection in a woman who is expecting a baby. The infection primarily affects the liver, causing inflammation and possible long-term complications such as cirrhosis or liver cancer (CDC, 2023). During pregnancy, the main concerns include maternal health risks and the possibility of transmitting the virus to the baby known as vertical transmission.
Unlike hepatitis B, there is currently no vaccine for hepatitis C. However, the rate of transmission during pregnancy is relatively low, around 5-7% (WHO, 2023). Risk factors that increase the likelihood of mother-to-child transmission include a high viral load and HIV infection. Most babies born to mothers with hepatitis C are not infected, but careful monitoring is necessary.
Treatment with direct-acting antivirals (DAAs) is usually delayed until after delivery, as safety data in pregnancy are limited. Supportive care, close monitoring, and planned provision with a healthcare provider are essential.
Understanding Hepatitis C in Pregnancy
Hepatitis C is caused by the hepatitis C virus (HCV), which is primarily transmitted through blood-to-blood contact. In pregnancy, the virus presents two challenges: protecting the mother’s health and preventing transmission to the baby.
Globally, approximately 71 million people live with chronic hepatitis C, and an estimated 3-4 million pregnant women are infected each year (WHO, 2023).
The majority of infected pregnant women are asymptomatic, meaning they do not even know they are carrying the virus.
Causes and risk factors in pregnancy
How hepatitis C is contracted.
Pregnant women can get hepatitis C in the same ways as the general population:
- Sharing needles or syringes
- Unsafe medical procedures (unsterile injections before 1992, blood transfusions)
- Tattooing or piercing with unsterile equipment
- Sexual transmission (less common, but higher if HIV is present)

Risk factors for transmission to the baby
The chance of transmitting hepatitis C to the newborn during pregnancy is approximately 5-7% (CDC, 2023). This risk increases when:
- The mother has a high viral load (>1 million IU/mL)
- The mother is co-infected with HIV
- There are complications during labor and delivery, such as prolonged rupture of membranes
Doctor’s insight: In my experience, mothers often assume that a C-section is mandatory if they have hepatitis C. However, research shows that cesarean delivery does not significantly reduce the risk of transmission. What is more important is careful labor management and avoidance of invasive procedures such as fetal skull monitoring.
Symptoms of hepatitis C in pregnancy
Symptoms of hepatitis C in pregnancy is a little confusing because most pregnant women with hepatitis C do not show any symptoms and, When symptoms do appear, they can mimic the common discomforts of pregnancy, making diagnosis difficult.
Common symptoms
- Fatigue (often mistaken for pregnancy fatigue)
- Nausea and poor appetite
- Jaundice (yellowing of the skin/eyes less common)
- Dark urine or pale stools
Read in Detail: [First Sign of Hepatitis C]
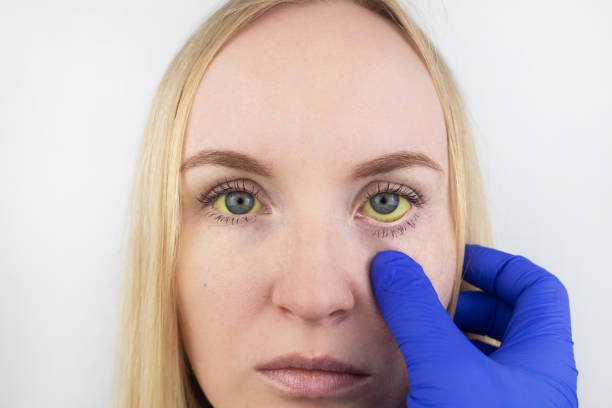
Rare but serious symptoms
- Severe itching due to cholestasis of pregnancy
- Abdominal pain or swelling (possible advanced liver disease)
For more details on the specific characteristics of men, see my blog: [Symptoms of Hepatitis C in Men].
7 Shocking Risks of Hepatitis C in Pregnancy
1. Mother-to-child transmission
The greatest risk of hepatitis C during pregnancy is the possibility of the virus being passed on to the baby during childbirth. On average, 5-7% of infants born to infected mothers are infected (CDC, 2023). Although most babies survive, this possibility poses significant concerns for expectant mothers. Careful monitoring during pregnancy and after birth is essential.
Doctor’s note: I reassure my patients that although this risk exists, the vast majority of babies do not contract the virus. Early testing and follow-up are key to peace of mind.
2. Increased risk of gestational diabetes
Research has shown that women with hepatitis C are more likely to develop gestational diabetes than uninfected mothers (PubMed, 2022). This condition can lead to complications such as a larger-than-average baby, a difficult delivery, and an increased risk of cesarean section. Managing blood sugar levels through diet and monitoring is very important for both mother and baby.
Doctor’s Note: I often remind mothers that diet and light exercise can make a big difference during pregnancy. Even small lifestyle adjustments can keep blood sugar under control.
3. Premature delivery
Hepatitis C in pregnancy has been linked to an increased risk of preterm delivery, meaning the baby is born before 37 weeks of gestation. Premature babies may experience breathing difficulties, breastfeeding problems, and longer stays in the neonatal intensive care unit (NICU). Early diagnosis and specialized prenatal care help reduce this risk.
Doctor’s Note: In my practice, when I suspect a risk of preterm labor, I work closely with the obstetrician to ensure that the mother has access to a hospital with a strong neonatal care unit. Preparation saves lives.
4. Low birth weight
Babies born to mothers with hepatitis C are more likely to have low birth weight. A baby weighing less than 2.5 kilograms at birth may have developmental delays and require additional medical care. This complication is often associated with premature birth and poor maternal health, emphasizing the importance of close follow-up during pregnancy.
Doctor’s Note: I encourage expectant mothers to focus on a balanced diet and regular prenatal visits. Monitoring fetal development via ultrasound is crucial to ensure timely intervention.
5. Intrahepatic cholestasis of pregnancy (ICP)
Hepatitis C significantly increases the risk of a liver condition called intrahepatic cholestasis of pregnancy (Mayo Clinic, 2023). ICP causes severe itching, especially at night, and if left untreated, can increase the risk of stillbirth. Women with both HCV and ICP require special care, including frequent liver tests and sometimes early delivery to protect the baby.
Doctor’s note: Many women describe itching as a common symptom of pregnancy. I advise my patients: If itching is severe or persistent, especially on the palms and soles, get checked out right away.
6. High cesarean section rate
Although hepatitis C alone does not medically require a C-section, many women with HCV deliver by cesarean section. This may be due to related complications such as gestational diabetes, preterm labor, or concerns about transmission. While not harmful, unnecessary surgeries carry additional risks such as infections and a longer recovery period.
Doctor’s Note: I make sure my patients know that vaginal delivery is safe in most cases of hepatitis C. The decision should always be medical, not fear-based.
7. Decreased maternal health
Pregnancy naturally puts stress on the liver, and if the mother already has hepatitis C, it can worsen liver inflammation or accelerate existing liver disease. In rare cases, women can experience complications such as cirrhosis or fluid retention. This highlights the importance of regular monitoring and timely postpartum treatment.
Doctor’s Note: I have seen how the stress of pregnancy can expose hidden liver problems. Regular blood tests help detect problems early, allowing for safe management for both mother and baby.
Diagnosis of hepatitis C in pregnancy
Screening recommendations
The CDC now recommends universal screening of all pregnant women for hepatitis C at least once during each pregnancy (CDC, 2023).
Blood tests: HCV antibody → confirmed by HCV RNA test.
Monitoring during pregnancy
- Liver function tests are done every trimester.
- Viral load monitoring
- Ultrasound if liver disease is advanced.
Treatment of hepatitis C during pregnancy
Treatment of hepatitis C during pregnancy is a bit challenging as currently, the gold standard treatment direct-acting antivirals (DAAs) is not approved for use in pregnancy due to limited safety data (WHO, 2023).
What can be done during pregnancy?
- Supportive care (nutrition, liver function monitoring)
- Vaccination against hepatitis A and B if not immune.
- Management of complications such as gestational diabetes
Postpartum treatment
After birth, mothers should have a complete check-up and can start DAAs, which can cure hepatitis C in more than 95% of cases.
Related: [Liver Cleanse Diet Plan] — Helpful for postpartum liver health.
Delivery and breastfeeding.
Method of Delivery
The good news for mothers with hepatitis C during pregnancy is that vaginal delivery is generally safe. Studies show that cesarean section (C-section) does not significantly reduce the risk of mother-to-child transmission (CDC, 2023). Instead, what matters most is careful labor management: avoiding invasive procedures such as fetal scalp electrodes, minimizing prolonged rupture of membranes, and ensuring a smooth delivery.
However, if there are other medical reasons such as placenta previa, fetal distress, or complications of gestational diabetes, a C-section may be recommended. In these cases, the decision is based on maternal health rather than hepatitis C infection.
Breastfeeding
Most women with hepatitis C can safely breastfeed their babies. Research shows that the virus is not transmitted through breast milk (WHO, 2023). The only exceptions are situations where the mother has cracked or bleeding nipples, which could expose the baby to infected blood. If the mother also has HIV, special precautions may be needed, and the pediatrician will provide guidance on breastfeeding.
Breastfeeding provides important benefits for the baby, including strong immunity, better digestion, and emotional bonding. Unless your doctor advises otherwise, breastfeeding should be encouraged.
Doctor’s note: I always remind new mothers that breastfeeding is not only safe but extremely beneficial, even with hepatitis C. If the nipples are sore or bleeding, I recommend temporarily pumping and stopping until they heal, then safely resuming breastfeeding.
Preventing Hepatitis C in Pregnancy
Since there is no vaccine, prevention is key:
- Avoid sharing needles or sharps.
- Ensure safe blood transfusions and medical procedures
- Use barrier protection if partner is HCV positive.
- Create a pregnancy care plan with a hepatologist and obstetrician
Read in Detail: [How to keep your liver healthy]
Diagnosis for mother and baby
Most mothers with hepatitis C in pregnancy give birth to healthy babies. Long-term outcomes depend on:
- Maternal viral load
- Presence of co-infection
- Timely diagnosis and postpartum treatment
Doctor’s note: In my practice, I have seen many mothers panic at the diagnosis. Reassurance is important: The majority of newborns do not acquire the infection, and mothers can recover after pregnancy.
Conclusion and Call to Action
Hepatitis C in pregnancy is a serious but manageable condition. With proper screening, monitoring, and postpartum treatment, both mother and baby can thrive.
If you are pregnant or planning to become pregnant and are concerned about hepatitis C, don’t panic. Talk to your doctor, get tested, and make sure you have the right care plan in place.
Have questions about hepatitis C in pregnancy? Leave them in the comments below – I’d be happy to guide you.
References:
WHO Hepatitis C in Pregnancy Fact Sheet
FAQS
Data is mixed. While some studies suggest a slight increase in risk, most women carry pregnancies successfully to term (PubMed, 2021).
Not during pregnancy, as DAAs aren’t approved. But after delivery, cure rates with DAAs exceed 95% (WHO, 2023).
No, breastfeeding is safe unless nipples are cracked/bleeding, or if you also have HIV (CDC, 2023).
No clear evidence shows C-sections reduce HCV transmission. The decision should be based on obstetric needs.
Yes, the CDC recommends universal screening at least once per pregnancy (CDC, 2023).
🧑⚕️ About the Author
Dr. Asif, MBBS, MHPE
Dr. Asif is a licensed medical doctor and qualified medical educationist with a Master’s in Health Professions Education (MHPE) and 18 years of clinical experience. He specializes in gut health and mental wellness. Through his blogs, Dr. Asif shares evidence-based insights to empower readers with practical, trustworthy health information for a better, healthier life.
⚠️ Medical Disclaimer
This blog is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard or delay medical advice based on content you read here.


Leave a Reply