Introduction
Hemorrhoids Relief Matters?
As a practicing physician, I often see patients who present with painful swelling, itching, or bleeding around the anus. Many people delay seeking help out of embarrassment, but the truth is that hemorrhoids (piles) are one of the most common anorectal conditions, affecting nearly half of adults by the age of 50.
The good news? Hemorrhoids can be effectively managed with lifestyle changes, home remedies, medications, and in some cases, medical procedures. In this comprehensive guide, I’ll tell you everything you need to know about hemorrhoid relief from causes of hemorrhoids, symptoms of hemorrhoids,types of hemorrhoids to medical treatment for hemorrhoids and its prevention. I’ll also share clinical experiences and practical tips that have helped my patients.
What are hemorrhoids?
Definition:
Hemorrhoids (commonly called “piles”) are vascular structures located in the anal canal that help cushion the passage of stool. They become a medical problem when they become swollen, inflamed, or elongated, causing pain, itching, bleeding, or discomfort.
Pathophysiology of Hemorrhoids
The anal canal contains a rich network of arteriovenous channels and connective tissue, known as the hemorrhoidal plexus.
Normally, these vascular cushions help maintain fine control of continence, especially preventing the passage of mucus or gas.
Hemorrhoids develop when venous pressure increases and the supporting tissue deteriorates, leading to:
- Involvement of the venous cushion
- Venous stasis and dilatation
- Protrusion of hemorrhoidal tissue through the anal canal
- Inflammation and thrombosis (formation of a clot in an external hemorrhoid)
Key mechanisms:
- Increased intra-abdominal pressure (constipation, pregnancy, obesity, prolonged sitting)
- Degeneration of collagen and elastic tissue with age
- Impaired venous return in the anorectal region.
Types of hemorrhoids
The main types of hemorrhoids include:
1. Internal hemorrhoids
- Start above the dentate (pectinate) line.
- Covered by columnar epithelium (no pain receptors → usually painless).
Key symptoms: painless rectal bleeding, distension, mucus discharge.
Classification of internal hemorrhoids (Gulliger classification):
- Grade I: no dilation; May bleed.
- Grade II: Prolapse during exertion but spontaneously reduces.
- Grade III: Prolapse requires manual reduction.
- Grade IV: Irreversible prolapse, strangulation risk.
2. External hemorrhoids
- Start below the dentate line.
- Covered with anoderm (skin with pain receptors) → Very painful when thrombosed.
Symptoms: swelling, pain, itching, difficulty sitting.
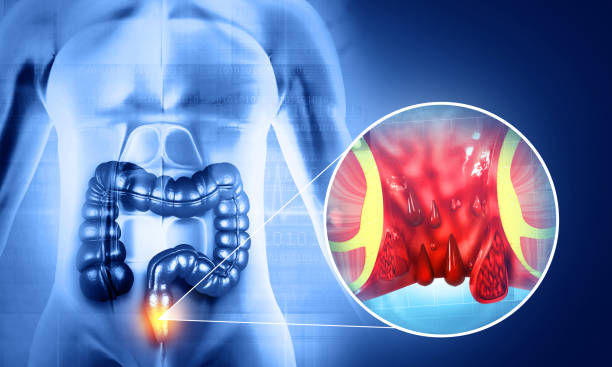
3. Thrombosed hemorrhoids
- A blood clot forms inside an external hemorrhoid, causing sudden severe pain and a blue lump.
- Often requires immediate treatment (incision/drainage or conservative management depending on the duration).
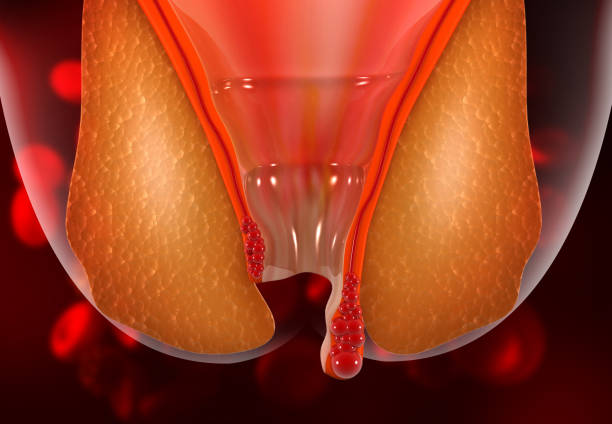
4. Prolapsed hemorrhoids
- Internal hemorrhoids that descend outside the anal opening.
- Can cause discomfort, difficulty with hygiene, and secondary skin irritation.
Epidemiological and statistical data
- Global prevalence: Hemorrhoids affect an estimated 4–35% of the population, depending on diagnostic criteria (Johansson & Sonnenberg, Gastroenterology, 1990).
- US data: Approximately 1 in 20 Americans and half of adults over 50 will experience hemorrhoids (NIH – National Institute of Diabetes and Digestive and Kidney Diseases, NIDDK).
- Hospital visits: Hemorrhoids account for more than 3.5 million doctor visits in the US annually (Everhart & Rohl, Digestive Diseases and Sciences, 2009).
- Age factor: Peak incidence occurs between 45-65 years.
- Gender: Both men and women are affected equally, but pregnancy increases the risk in women.
Causes of Hemorrhoids
Based on the patient cases I’ve seen, the most common causes of hemorrhoids include:
- Chronic constipation or straining during bowel movements
- Low-fiber diet
- Prolonged sitting, especially on the toilet
- Obesity
- Pregnancy and vaginal delivery
- Aging and weakening of the rectal tissues
- Family history of hemorrhoids
Symptoms of hemorrhoids
Common symptoms of hemorrhoids include:
- Bright red blood during or after a bowel movement
- Itching and burning around the anus
- Swelling or lump near the anus
- Pain or discomfort, especially when sitting
- Mucus discharge (in long hemorrhoids)
Note: Bleeding should never be ignored. In my clinical experience, a few patients assumed it was “just hemorrhoids,” but were later diagnosed with colon cancer.
Learn here how to differentiate hemorrhoids vs. colon cancer symptoms (“Hemorrhoids vs. Colon Cancer Symptoms”)
Diagnosis: How Doctors Confirm Hemorrhoids.
Many people assume that rectal bleeding or discomfort is “just hemorrhoids,” but as a doctor, I can’t stress this enough: Not all rectal bleeding is caused by hemorrhoids. Other conditions like fissures, polyps, or even colorectal cancer can mimic these same symptoms. That’s why an accurate diagnosis is essential.
Here’s how doctors typically confirm hemorrhoids:
Review of medical history and symptoms
Doctors will ask about bowel habits, diet, constipation, bleeding, pain, and family history of colon diseases.
Example: I often ask patients, “Do you see blood only on the toilet paper, or is it mixed with your stool?” This distinction helps rule out more serious conditions.
Physical exam
For external hemorrhoids, the doctor can often see or feel a swollen, tender lump near the anus.
Thrombosed hemorrhoids are usually blue, firm, and painful.
Digital rectal exam (DRE)
A gloved, lubricated finger is gently inserted into the rectum.
This helps detect internal hemorrhoids, masses, or abnormal growths.
Anoscopy
A small lighted tube is inserted into the anus to view internal hemorrhoids.
This is often a quick and easy office procedure.
Proctoscopy/Sigmoidoscopy/Colonoscopy
If the bleeding is heavy or persistent, the doctor may recommend these procedures to examine the inside of the large intestine.
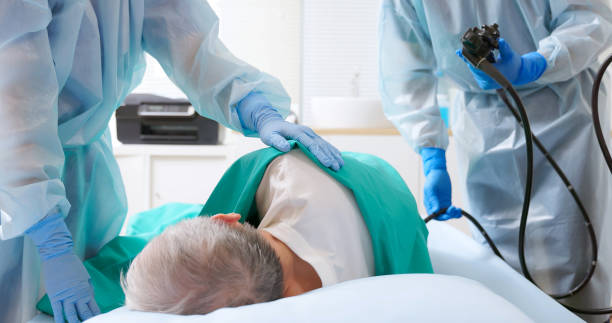
Colonoscopy is especially important in patients over 40 years of age or those with a family history of colon cancer.
Key Clinical Notes:
I have had patients who have delayed a colonoscopy, assuming “it’s just a pile,” but further testing revealed polyps or early-stage cancer. That’s why diagnosis should never be put off.
Hemorrhoids Relief: Treatment Options
1. Home Remedies for Hemorrhoids Relief
Many patients prefer to start with natural measures for Hemorrhoids relief. The most effective treatments I recommend are:
- Warm sitz baths: Sitting in warm water 2-3 times daily reduces swelling and pain.
- Fiber-rich diet: Include fruits, vegetables, legumes, and whole grains.
- Stay hydrated: Drink at least 8-10 glasses of water daily.
- Basic natural agents: Witch hazel, aloe vera gel, and coconut oil relieve itching.
- Ice packs: Reduce swelling and numbing pain.
- Avoid stress: Go to the bathroom when the urge comes, don’t force a bowel movement.
Read Natural Remedies for Hemorrhoids Here (“Natural Remedies for Hemorrhoids“)
2. Over-the-Counter (OTC) Treatments for Hemorrhoids Relief
For immediate Hemorrhoids relief, patients often turn to:
- Hemorrhoid creams and suppositories (hydrocortisone-based)
- Pain relievers like acetaminophen or ibuprofen
- Wipe with witch hazel instead of dry toilet paper.
Medical Treatment for Hemorrhoids
When home remedies and lifestyle changes don’t bring enough relief, medical treatment for Hemorrhoids is the next step. Treatments vary depending on the severity, type, and consistency of the hemorrhoids.
Here are the main medical treatment for Hemorrhoids that doctors use:
1. Rubber Band Ligation (Banding)
How it works: A small rubber band is placed at the base of the internal hemorrhoid. This cuts off the blood supply, causing it to shrink and fall off in 5-7 days.
Best for: Internal hemorrhoids (grades I–III).
Pros: Outpatient procedure, effective in most cases.
Cons: Some discomfort, light bleeding, rare infection.
2. Sclerotherapy
How it works: A chemical solution is injected into the hemorrhoid tissue, causing it to shrink.
Best for: Small to medium internal hemorrhoids.
Pros: Quick, minimally invasive.
Cons: Less effective for larger hemorrhoids, repeat sessions may be required.
3. Infrared Coagulation (IRC)
How it works: A beam of infrared light is applied to the hemorrhoid tissue, cutting off blood flow and causing it to shrink.
Best for: Early stage internal hemorrhoids.
Pros: Painless, quick recovery.
Cons: May not work for larger hemorrhoids. Recurrence is possible.
4. Electrocoagulation (diathermy)
How it works: Uses electric current or heat to coagulate the blood vessels inside the hemorrhoid.
Best for: Internal hemorrhoids.
Pros: Effective for controlling bleeding.
Cons: Slight risk of pain or ulceration.
5. Hemorrhoidectomy (surgical removal)
How it works: Hemorrhoid tissue is surgically removed.
Best for: Severe, large, long, or thrombosed hemorrhoids that don’t respond to other treatments.
Pros: Permanent solution.
Cons: Recovery can be painful, healing time 2-4 weeks, risk of infection or narrowing of the anal canal.
6. Stapled hemorrhoidopexy (PPH – procedure for prolapsed and hemorrhoids)
How it works: Hemorrhoids are stapled back into place inside the rectum, cutting off blood flow and slowing growth.
Best for: Prolapsed internal hemorrhoids.
Pros: Less painful than hemorrhoidectomy, quicker recovery.
Cons: Slightly higher recurrence rate than traditional surgery.
7. Doppler-guided hemorrhoidal artery ligation (HAL-RAR)
How it works: Uses ultrasound (Doppler) to locate the hemorrhoid arteries, which are then occluded to reduce blood supply.
Best for: Internal hemorrhoids and bleeding.
Pros: Less painful, preserves anal tissue.
Cons: Expensive, may not be widely available.
8. Treating Thrombosed External Hemorrhoids
If diagnosed early (within 48-72 hours), doctors can perform an incision and drainage to remove the clot and relieve pain.
If left untreated, the clot may resolve within weeks, but the pain is usually severe at first.
9. Medications for Hemorrhoids Relief that your doctor may prescribe:
- Topical corticosteroids (hydrocortisone) – reduce swelling and itching.
- Topical anesthetics (lidocaine, pramoxine) – for pain relief.
- Oral flavonoids (diosmin, hesperidin) – strengthen veins, thin blood (widely used in Europe/Asia).
- Stool softeners – prevent hemorrhoids from straining and getting worse.
Hemorrhoids Relief in pregnancy
Pregnant women are especially prone to this due to hormonal changes, constipation, and increased pressure on the pelvic veins.
For pregnancy-related hemorrhoids, I recommend:
- Eat a light, high-fiber diet.
- Drink plenty of water.
- Use safe stool softeners if prescribed.
- Apply cold compresses to swelling.
- Avoid prolonged sitting.
👉 Read the full blog on hemorrhoids in pregnancy here.
Long-Term Hemorrhoids Relief: How to Prevent Hemorrhoids
While treatment can provide relief, the best way to manage hemorrhoids is to prevent them from coming back. In my clinical experience, patients who commit to a healthy lifestyle rarely experience recurring episodes. Here’s how you can protect yourself in the long run:
1. Eat 25-30 grams of fiber daily.
A diet rich in fiber softens stool and increases bulk, which reduces straining during bowel movements the leading cause of hemorrhoids.
The best sources of fiber include:(Read complete Article About Fiber Rich Food)
- Whole grains: oats, brown rice, barley
- Fruits: apples, pears, plums
- Vegetables: broccoli, spinach, carrots
- Legumes: beans, lentils, chickpeas
- Nuts and seeds: flaxseeds, chia seeds, almonds
It’s important to increase fiber gradually to avoid bloating or gas. If diet alone isn’t enough, fiber supplements like psyllium husk (Metamucil) or methylcellulose can help.
2. Stay well hydrated
Water works in conjunction with fiber. Without adequate hydration, fiber can actually worsen constipation.
- Aim to drink 8-10 glasses of water daily.
- Herbal teas and clear soups can also help with fluid intake.
- Limit caffeine and alcohol, which can dehydrate you.
A simple rule I tell my patients: “If your urine is light yellow, you are hydrated enough.”
3. Exercise regularly.
Physical activity stimulates bowel function, reduces constipation and stress. It also prevents obesity, which is a risk factor for hemorrhoids.
Good options include:
- Brisk walking (30 minutes a day)
- Swimming
- Yoga (poses like Malasana/squatting are great for bowel health)
- Cycling (with proper seat padding to avoid pressure on the anus)
Avoid lifting heavy weights with pressure, as this can worsen hemorrhoids.
4. Don’t sit on the toilet for too long.
Many patients develop hemorrhoids from scrolling too much on their phones while on the toilet. Sitting for too long increases pressure on the veins in the rectum.
Tips:
- Go only when you feel a natural urge.
- Limit time sitting on the toilet to <5 minutes.
- Avoid straining or straining unnecessarily.
5. Manage stress and avoid stress for Hemorrhoids Relief
Stress can indirectly worsen hemorrhoids by contributing to symptoms like constipation, poor eating habits, or IBS.
- Practice deep breathing, meditation, or relaxation exercises.
- Stick to a sleep and eating routine.
- Address anxiety related digestive issues with professional help if needed.
6. Maintain a healthy weight
Excess weight, especially around the abdomen, increases pressure on the rectal veins and contributes to the formation of hemorrhoids.
- Aim for a balanced diet with controlled portions.
- Combine cardio and strength training for gradual weight loss.
Even a 5-10% weight loss can significantly reduce the risk of hemorrhoids in overweight patients.
Final Clinical Note
Patients who consistently follow these precautions often tell me, “Dr., my bowel habits have improved so much that I don’t even think about hemorrhoids anymore.”
Prevention is not only about avoiding discomfort, but also about improving overall digestive health.
If you’ve had hemorrhoids before, adopting these steps can dramatically reduce the rate of recurrence.
Complications of untreated hemorrhoids
Ignoring hemorrhoids can lead to:
- Anemia (chronic blood loss)
- Strangulated hemorrhoids (blood supply cut off, causing severe pain)
- Infection
- Impact on quality of life (persistent pain, embarrassment, or hygiene problems)
My clinical experience with hemorrhoid patients
A 45-year-old man delayed treatment for rectal bleeding, thinking it was hemorrhoids. Further testing revealed that she had hemorrhoids and early-stage colon cancer. Early intervention saved her life.
A young woman developed painful external hemorrhoids after giving birth. With sitz baths, fiber, and topical treatments, she recovered without surgery.
These stories highlight the importance of not ignoring symptoms and getting a prompt diagnosis from a doctor.
American Society of Colon and Rectal Surgeons – Hemorrhoids
Mayo Clinic – Hemorrhoids: Symptoms and Causes
Conclusion and Call to Action
Hemorrhoids are common but treatable. Whether you’re dealing with mild discomfort or severe symptoms, there are several ways to find lasting hemorrhoids relief.
From simple lifestyle changes like eating more fiber to medical treatments and surgery, relief is possible at every stage.
FAQS
Yes, you can significantly reduce your risk of developing hemorrhoids by:
- Eating a high-fiber diet (fruits, vegetables, whole grains).
- Drinking plenty of water to keep stools soft.
- Avoiding straining during bowel movements.
- Going to the bathroom as soon as you feel the urge.
- Exercising regularly to prevent constipation.
For more persistent or severe hemorrhoids, a doctor may recommend:
- Rubber band ligation: A small rubber band is placed around the base of the hemorrhoid to cut off its blood supply, causing it to shrink and fall off.
- Sclerotherapy: A chemical solution is injected into the hemorrhoid to shrink it.
- Coagulation (infrared, laser, or bipolar): Using heat to destroy the hemorrhoid tissue.
- Surgical removal (hemorrhoidectomy): This is a highly effective option for large, severe, or recurrent hemorrhoids.
For mild cases, you can find relief with:
- Sitz baths: Soaking the anal area in warm water for 10-15 minutes, two to three times a day.
- Over-the-counter creams and ointments: Products containing witch hazel or hydrocortisone can help soothe itching and pain.
- Fiber supplements: Psyllium husk (like Metamucil) can help soften stools.
- Cold compresses or ice packs: Applying them to the affected area for short periods can help reduce swelling and pain.
Symptoms can vary depending on whether the hemorrhoids are internal or external.
- External hemorrhoids: Itching or irritation in your anal region, pain or discomfort, swelling around your anus, and sometimes bleeding.
- Internal hemorrhoids: Painless bleeding during bowel movements (you might see bright red blood on the toilet paper), and a prolapsed or protruding hemorrhoid, which can cause pain and irritation.
Hemorrhoids are often caused by increased pressure in the lower rectum. Common causes include:
- Straining during bowel movements
- Chronic constipation or diarrhea
- Sitting on the toilet for long periods
- Obesity
- Pregnancy
- A low-fiber diet
🧑⚕️ About the Author
Dr. Asif, MBBS, MHPE
Dr. Asif is a licensed medical doctor and qualified medical educationist with a Master’s in Health Professions Education (MHPE) and 18 years of clinical experience. He specializes in gut health and mental wellness. Through his blogs, Dr. Asif shares evidence-based insights to empower readers with practical, trustworthy health information for a better, healthier life.
⚠️ Medical Disclaimer
This blog is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard or delay medical advice based on content you read here.

Leave a Reply