Introduction
Difference Between Fatty Liver and Cirrhosis – Why It Matters.
As a practicing physician and medical educator, I have encountered many patients who are confused about the difference between fatty liver and cirrhosis. While both involve liver damage, their causes, reversibility, and long term outcomes are very different.
Unfortunately, liver disease often progresses silently, and by the time symptoms appear, it may be too late to reverse the damage. Therefore, understanding these conditions is important not only for those who have already been diagnosed but also for those who want to prevent liver problems altogether.
In this article, I will explain the difference between fatty liver and cirrhosis using clinical experience, real data, and patient friendly language. We will also discuss early symptoms, diagnostic methods, and lifestyle interventions that can make a real difference.
What is fatty liver disease?
(Also known as hepatic steatosis)
Fatty liver disease occurs when excess fat builds up in the liver. It is broadly classified as:
- NAFLD (Non-alcoholic fatty liver disease) – seen in people who drink little or no alcohol.
- AFLD (Alcoholic fatty liver disease) – caused by excessive alcohol consumption.
Causes of fatty liver:
- Obesity or overweight
- Type 2 diabetes
- High cholesterol or triglycerides
- Sedentary lifestyle
- Unhealthy diet (especially processed sugars and fats)
- Certain medications (such as corticosteroids, methotrexate)
Symptoms:
In most cases, fatty liver is asymptomatic. When symptoms do appear, they are usually vague:
- Fatigue
- Mild upper abdominal discomfort
- General malaise
Is fatty liver reversible?
Yes, with lifestyle changes, fatty liver can be reversed in its early stages.
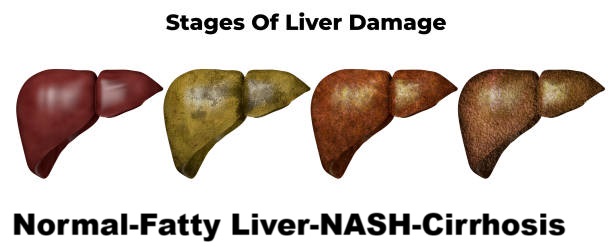
What is liver cirrhosis?
Cirrhosis is the final stage of chronic liver disease, where healthy liver tissue is replaced by scar tissue (fibrosis), causing permanent damage.
This scarring affects the liver’s ability to perform important functions such as filtering blood, making proteins, and storing nutrients.
Common causes of cirrhosis:
The common causes of Cirrhosis include:
- Chronic hepatitis B or C
- Long-term alcohol abuse
- Non-alcoholic steatohepatitis (NASH)
- Autoimmune liver diseases
- Genetic conditions (e.g., Wilson’s disease, hemochromatosis)
Symptoms of Cirrhosis:
Unlike fatty liver, symptoms of cirrhosis are more serious and visible , such as:
- Jaundice (yellowing of the skin and eyes)
- Swelling of the abdomen (swelling)
- Confusion (hepatic encephalopathy)
- Easy bruising or bleeding
- Spider-like blood vessels on the skin
- Loss of appetite and weight loss
Key Difference Between Fatty Liver and Cirrhosis
Here’s a clear comparison table showing the difference between fatty liver and cirrhosis:
| Feature | Fatty Liver | Cirrhosis |
|---|---|---|
| Cause | Fat accumulation | Long-term liver damage and scarring |
| Reversibility | Reversible with lifestyle change | Irreversible, only manageable |
| Symptoms | Often silent | Serious, visible signs |
| Progression | May progress to NASH & cirrhosis | Final stage of liver disease |
| Liver Function | Usually normal | Severely impaired |
| Treatment | Lifestyle & diet | Monitoring, medication, transplant in severe cases |
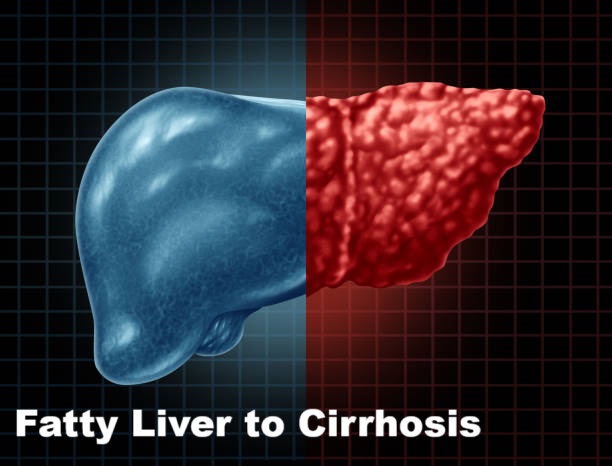
Overlap: How Fatty Liver Can Lead to Cirrhosis.
Many patients think these are unrelated conditions. In fact, if ignored, fatty liver can progress to cirrhosis.
Here’s how it typically plays out:
Fatty Liver (NAFLD/AFLD)—-NASH (Non-Alcoholic Steatohepatitis) —–Fat + Inflammation-Fibrosis ——Initial Scarring-Cirrhosis —–Permanent Liver Damage
According to a study published in PubMed, approximately 20-30% of patients with NASH develop cirrhosis over time (PubMed ID: 32898611).
This makes early diagnosis and lifestyle interventions extremely important.
Fatty Liver vs Cirrhosis Diagnosis
As a physician, I always emphasize the importance of early detection through simple tests:
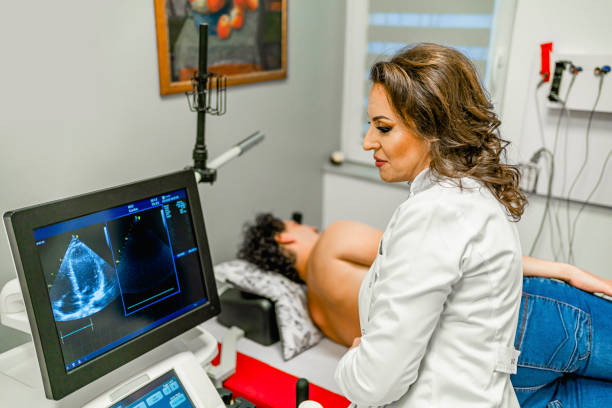
For Fatty Liver:
- Liver Ultrasound
- Liver Function Tests (ALT, AST)
- FibroScan (to assess severity)
For Cirrhosis:
- FibroScan or Liver Biopsy (to confirm stage)
- Blood Tests (low albumin, high INR)
- Imaging (CT/MRI)
- Endoscopy (to check for viruses)
Treatment of Fatty Liver vs cirrhosis
Treatment of Fatty Liver:
- Dietary Changes: Mediterranean Diet, Avoid Sugar, Refined Carbohydrates.
- Exercise: At least 150 minutes of moderate exercise weekly
- Weight loss: Even a 5-10% loss helps.
- Control diabetes, cholesterol, BP.
[Explanation of fatty liver disease Read Here]
Treat cirrhosis:
- Quit alcohol completely.
- Treat underlying cause: Hepatitis B/C antivirals, autoimmune treatments
- Manage complications: Diuretics for ascites, lactulose for encephalopathy
- Liver transplant in advanced cases
[ Read Hep B vaccine schedule for adults]
Real patient case: A wake-up call
I once treated a 42-year-old teacher with a routine health checkup who had mildly elevated liver enzymes. Ultrasound confirmed fatty liver. Despite repeated consultations, he delayed making lifestyle changes. Within 6 years, he returned with fatigue, abdominal swelling, and jaundice a diagnosis of cirrhosis.
This case highlights how fatty liver is a silent warning, and ignoring it can lead to irreversible damage.
Unique Insight: Why Cirrhosis Is Often Missed Until Late.
In my clinical experience, many patients mistake bloating or mild fatigue for digestive problems, not realizing that it could be the liver’s skin rotting.
Furthermore, cirrhosis often remains in remission (no major symptoms) for years before complications develop. That’s why regular checkups and liver scans are essential, even if you feel fine.
Prevention: Protect your liver early.
Whether you’re at risk for fatty liver or cirrhosis, prevention is key. Here’s how to protect your liver:
- Eat whole, unprocessed foods.
- Limit or completely avoid alcohol.
- Exercise regularly.
- Maintain a healthy weight.
- Get vaccinated against hepatitis B.
[When to get Hepatitis B Vaccine Booster]
According to the CDC, hepatitis B vaccination can prevent 90 percent of chronic infections in adults, which is a leading cause of cirrhosis (CDC Hepatitis B).
Trusted resources for further reading
Final thoughts
The difference between fatty liver and cirrhosis isn’t just a matter of terminology it’s the difference between a potentially reversible condition and one that can be life threatening if ignored.
If you or a loved one has been diagnosed with fatty liver, take it seriously. It’s not “just fat” in the liver it’s a red flag. With early action, you can reverse the damage and avoid the complications of cirrhosis.
Call to Action
If you found this article helpful, please share it, leave a comment below, or ask a question you have. And if you’re dealing with any liver related symptoms, don’t delay see your doctor today. Your liver works hard for you take care of it in return.
FAQS
Yes, it can. While not everyone with fatty liver will develop cirrhosis, it is a significant risk factor. The progression often follows a path:
- Simple Steatosis (Fatty Liver): Fat accumulation with little to no inflammation.
- NASH (Non-alcoholic Steatohepatitis): Fat accumulation with inflammation and early scarring.
- Fibrosis: Increasing scarring.
- Cirrhosis: Extensive scarring that has replaced healthy liver tissue
Cirrhosis is not reversible. The scar tissue is permanent. However, treatment can slow down the progression of the disease and manage its complications. Treatment involves:
- Treating the underlying cause: Stopping alcohol use or managing a viral hepatitis infection.
- Managing complications: Medications for fluid retention, beta-blockers for high blood pressure in the liver, and regular screenings for liver cancer.
- Liver Transplant: In advanced cases of liver failure, a transplant may be the only option.
Yes, in many cases, fatty liver is treatable and even reversible, especially in its early stages. Treatment focuses on addressing the underlying cause:
- For NAFLD: Weight loss, a healthy diet, exercise, and managing conditions like diabetes and high cholesterol.
- For Alcoholic Fatty Liver: Complete abstinence from alcohol is crucial.
In its early stages, fatty liver often has no symptoms. If symptoms do occur, they are often mild and non-specific, such as fatigue or a dull ache in the upper right abdomen.
The key difference is the presence and extent of scarring. Fatty liver is an early, and often reversible, stage of liver disease defined by fat accumulation. Cirrhosis is a much more advanced, irreversible stage marked by extensive, permanent scarring of the liver. Think of fatty liver as a precursor to cirrhosis in many cases.
🧑⚕️ About the Author
Dr. Asif, MBBS, MHPE
Dr. Asif is a licensed medical doctor and qualified medical educationist with a Master’s in Health Professions Education (MHPE) and 18 years of clinical experience. He specializes in gut health and mental wellness. Through his blogs, Dr. Asif shares evidence-based insights to empower readers with practical, trustworthy health information for a better, healthier life.
⚠️ Medical Disclaimer
This blog is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard or delay medical advice based on content you read here.

Leave a Reply