Introduction
Causes of IBS in women are a topic that is often misunderstood, even among those who live with the condition every day. As a licensed physician and medical educator, I have seen countless women in my clinic who follow a healthy lifestyle but still experience bloating, abdominal pain, unpredictable bowel habits, and discomfort.
If this sounds familiar, you are not alone. Irritable Bowel Syndrome (IBS) affects women almost twice as often as men, according to Mayo Clinic data, and the triggers can be more complex than what’s on your plate. From hormonal fluctuations to stress and gut microbiome imbalances, the causes are deeply intertwined.
Let’s break it down in simple language as if you were sitting next to me in my consultation room.
What Are Causes Of IBS In Women
The causes of IBS in women involve a combination of biological, psychological, and lifestyle factors that interact with each other. The most common causes include hormonal fluctuations, gut-brain axis dysfunction, stress, dietary triggers, gut microbiome imbalances, and increased gut sensitivity.
Women are particularly susceptible to IBS symptoms because fluctuations in estrogen and progesterone affect bowel movement patterns, gut motility, and sensitivity. Emotional factors such as anxiety and stress can exacerbate these symptoms by disrupting nerve signals between the brain and gut.
Unlike structural gut diseases, IBS is considered a functional disorder, meaning the gut looks normal but does not function normally. Identifying the underlying causes helps personalize management strategies dietary adjustments, stress management, gut directed therapies, and medical intervention when needed.
In short: IBS in women is caused by multiple, overlapping factors not just diet which makes a holistic approach essential for long term relief.
Understanding IBS in women (why it’s so common).
IBS is one of the most prevalent gastrointestinal disorders worldwide. According to the World Health Organization (WHO), 10-15% of adults suffer from IBS, and women are twice as likely to be affected as men.
A quick look at how IBS works
Think of your digestive system as a highway system. In a healthy gut, traffic flows smoothly. But in IBS, the traffic signals (gut nerve signals) are erratic. This can lead to either traffic jams (constipation) or rush hour chaos (diarrhea), often alternating between the two.
Women’s gastrointestinal systems are particularly sensitive to hormonal changes, stress, and dietary triggers, making IBS symptoms more frequent and severe.
Read in Detail About: [Irritable Bowel Syndrome Explained]
Hormonal causes of IBS in women
Hormonal fluctuations are the strongest predictors of IBS symptom flare ups in women.
Estrogen and progesterone fluctuations
Estrogen and progesterone affect bowel motility the speed at which food moves through the intestines. High levels of progesterone during the luteal phase of the menstrual cycle can slow down bowel movements, leading to bloating and constipation. Conversely, a drop in estrogen during menstruation can increase bowel sensitivity and pain.
Unique Insight:
Many women report worsening IBS symptoms during their menstrual cycle. In clinical practice, tracking symptoms with menstruation often reveals clear hormonal patterns.
IBS and Menopause
Menopause brings another hormonal change, with lower estrogen levels that can disrupt bowel movements and microbial balance. Hot flashes, anxiety, and sleep disturbances during this phase can worsen IBS symptoms.
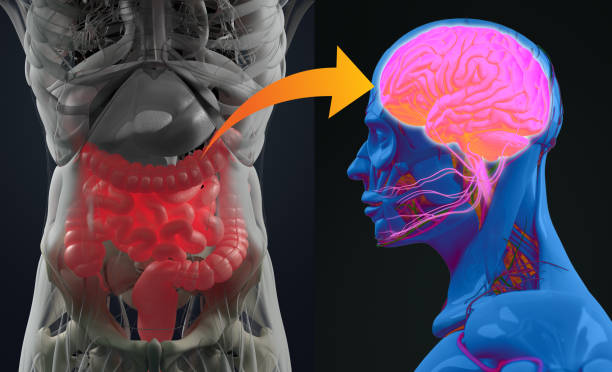
Gut Brain Axis Dysfunction (The Hidden Trigger)
The gut brain axis is a two way communication system between your brain and your digestive tract. When this system is overactive or dysregulated, IBS symptoms can worsen.
Stress and Anxiety
According to the CDC, more than 60% of women with IBS report stress as a major trigger. Emotional distress can increase gut sensitivity and alter motility, which can result in pain, bloating, or urgency.
Trauma and Emotional History
Research published in PubMed suggests that women with a history of trauma or chronic stress have higher rates of IBS. This is due to changes in stress hormones, such as cortisol, which affect bowel function over time.
Unique Insight:
In my clinical experience, patients who engage in stress management strategies such as breathing exercises, therapy, or gut directed hypnotherapy often see a reduction in flare ups even without dietary changes.
Read in Detail About: [Treatment for irritable bowel syndrome]
Microbiome imbalance (The hidden ecosystem)
Your gut is home to trillions of microorganisms, collectively called the gut microbiome. When this ecosystem is balanced, digestion runs smoothly. But when it’s disrupted due to antibiotics, illness, or diet IBS symptoms can flare up.
Dysbiosis and IBS
Studies show that women with IBS often have low levels of beneficial bacteria like Lactobacillus and Bifidobacterium. This imbalance can lead to increased gas, bloating, and inflammation.
Antibiotic Use and Hormonal Contraception
Repeated antibiotic use can wipe out good bacteria. Some hormonal contraceptives can also indirectly affect the composition of the gut microbiome.
Read in Detail About: [Best Probiotics for IBS Diarrhea]
Dietary Triggers of IBS
Diet is one of the most common aggravating factors for IBS but not always the root cause.Dietary triggers of IBS include:
High FODMAP Foods
Foods high in FODMAPs (Fermentable Oligo-, Di-, Mono-saccharides, and Polyols) and the most common dietary triggers of IBS. These include wheat, onions, garlic, apples, and dairy.

Lactose and Gluten Sensitivity
Many women with IBS have non celiac gluten sensitivity or lactose intolerance, which can mimic or worsen IBS symptoms.
Unique Insight:
While elimination diets can help identify triggers, they should be done under medical guidance. Overly restrictive diets can actually worsen long term gastrointestinal health.
Gut Sensitivity (When Your Gut Overreacts)
Even without overt inflammation, the intestines of IBS sufferers become hypersensitive.
Visceral Hypersensitivity
This means that the gut overreacts to normal amounts of gas or straining. Think of it like a microphone turned up too loud every sound (or sensation) feels amplified.
Hormonal Amplification in Women
Oestrogen may lower the threshold for pain perception, causing women to report more severe bloating and pain than men.
Psychological factors (Mind gut link)
Anxiety, depression and IBS
Women are more prone to anxiety and depression, both of which are closely related to IBS symptoms. A PubMed meta analysis found that up to 50% of IBS patients have coexisting anxiety or depression symptoms and depression and IBS are very closely related.
Vicious cycle of symptoms
IBS causes anxiety, and anxiety worsens IBS creating a feedback loop. Both gut directed and mind focused interventions are often needed to break this cycle.
Unique triggers of IBS in women
Most articles ignore these less obvious causes of IBS in women, but as a doctor, I see them often:
- Iron supplements can worsen constipation and bloating.
- Hormonal changes related to pregnancy changes in motility
- PCOS and thyroid dysfunction can increase the sensitivity of the intestines.
- Sleep disturbances associated with increased abdominal pain
- Post infectious IBS develops after food poisoning or a gut infection.
Unique insight:
I have treated several women whose IBS symptoms have improved dramatically after treating the underlying thyroid dysfunction.
Lifestyle factors (The impact of daily life)
Sedentary lifestyle
Lack of movement slows down bowel movements. Gentle activities like walking and yoga can make a real difference.
Irregular eating patterns
Skipping meals or eating too fast can trigger IBS symptoms by confusing the natural rhythm of your bowels.
Read in Detail About: [Best foods for irritable bowel syndrome]
Medical diagnosis (why diagnosis is important)
IBS is a diagnosis of exclusion, meaning other conditions must be ruled out.
When to see a doctor
If you have red flag symptoms weight loss, rectal bleeding, persistent pain, or anemia see your doctor right away.
Diagnostic tools
- Review of history and symptoms
- Blood tests
- Stool tests
- Colonoscopy (if indicated)
Read in Detail: [Diagnosis of irritable bowel syndrome]
References: Mayo Clinic – IBS Overview and WHO Digestive health
Practical steps to control the causes of IBS in women
While the causes of IBS in women cannot always be eliminated, they can be effectively managed.
Evidence Based Strategies
- Tract symptoms with a diary (especially during your period)
- Identify food triggers with a structured plan.
- Manage stress with breathing, therapy, or mindfulness.
- Support your microbiome with probiotics and a fiber rich diet.
- Consult your doctor for a hormonal and thyroid evaluation.
Real Patient Story
Sarah, a 32 year old teacher, came to me with severe bloating and alternating constipation. By tracking her symptoms along her cycle and adjusting her diet, as well as introducing light exercise and probiotics, her symptoms improved within three months without harsh medications.
Read in Detail About: [Treatment for Irritable Bowel Syndrome]
Final Thoughts – Taking Control of Your Gut Health
The causes of IBS in women are complex, involving hormones, gut brain communication, microbiome balance, diet, and lifestyle factors. But the good news is that with the right understanding and guidance, symptoms can be significantly reduced or prevented.
Remember:
- IBS does not define your health.
- Understanding your body is the first step toward healing.
- Small, consistent changes often bring big relief.
Call To Action:
If you’re struggling with persistent IBS symptoms, don’t ignore them.
Comment below about your experience or Book a consultation to discuss your personalized management plan. Your gut health deserves care and attention.
FAQS
Yes, in some women, hormonal contraceptives can indirectly influence gut function and microbiome composition, leading to bloating or altered bowel habits.
Stress affects the gut-brain axis, increasing sensitivity and altering digestion speed. Relaxation techniques can significantly reduce flare-ups.
IBS doesn’t damage the intestines or increase cancer risk, but it can affect quality of life. Medical evaluation is important to rule out other conditions.
High FODMAP foods like onions, garlic, wheat, apples, and dairy can worsen symptoms. But triggers vary, so a personalized plan works best.
Women have hormonal cycles that affect gut motility and sensitivity. Estrogen and progesterone fluctuations, combined with stress and lifestyle factors, make IBS more common in women.
🧑⚕️ About the Author
Dr. Asif, MBBS, MHPE
Dr. Asif is a licensed medical doctor and qualified medical educationist with a Master’s in Health Professions Education (MHPE) and 18 years of clinical experience. He specializes in gut health and mental wellness. Through his blogs, Dr. Asif shares evidence-based insights to empower readers with practical, trustworthy health information for a better, healthier life.
⚠️ Medical Disclaimer
This blog is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard or delay medical advice based on content you read here.



Leave a Reply