Introduction
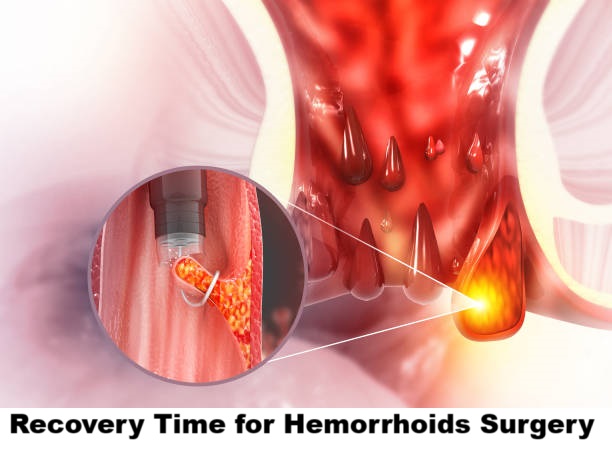
Hemorrhoids surgery recovery time is one of the most common concerns for patients preparing to have hemorrhoids removed. As a physician, I have seen how knowing what to expect after surgery can reduce anxiety and improve recovery outcomes.
Hemorrhoids swollen veins in the rectum or anal area are common, and while many respond to lifestyle changes and medications, some require surgery for lasting relief. Understanding the hemorrhoids surgery recovery time, potential complications,duration of hemorrhoid surgery and the best surgical procedure for your condition can help you make informed decisions.
When is surgery indicated for hemorrhoids?
Hemorrhoid surgery is considered only when conservative measures (dietary changes, medications, office procedures) fail to control symptoms or when complications develop. The decision also depends on the type and severity of hemorrhoids.
Types of hemorrhoids
- Internal hemorrhoids – occur inside the rectum and are usually painless but may bleed, enlarge, or cause mucus discharge. They are graded I through IV based on severity.
- External hemorrhoids – occur under the skin around the anus, often painful, especially when thrombosed (a blood clot forms inside).
- Mixed hemorrhoids – have both internal and external components, which may require combined surgical treatment.

Indications for surgery in internal hemorrhoids
Hemorrhoid Surgery is recommended for internal hemorrhoids when:
- Grade III or IV hemorrhoids (long and cannot be reduced manually).
- Severe bleeding due to anemia.
- Recurrent prolapse despite office procedures such as rubber band ligation.
- Failed nonsurgical treatments (diet, fiber supplements, topical medications, Read remedies that help in hemorrhoids here).
- Complications such as strangulated hemorrhoids or ulceration.
Indications for surgery in external hemorrhoids
Hemorrhoid Surgery may be required for external hemorrhoids when:
- Large, symptomatic hemorrhoids cause persistent pain, itching, or hygiene problems.
- Thrombosed hemorrhoids cause severe pain and swelling that does not improve within 48-72 hours.
- Chronic inflammation or recurrent flare-ups interfere with daily activities.
- After multiple recurrences, the patient prefers a permanent solution.
Clinical Insight:
In my practice, patients with recurrent thrombosed external hemorrhoids often report significant improvements in quality of life after surgical removal.
Duration of hemorrhoid surgery
The duration of hemorrhoid surgery depends on the type:
- Traditional Hemorrhoidectomy: 30-60 minutes.
- Stapled Hemorrhoidopexy: 20-40 minutes.
- Laser Hemorrhoidoplasty: 15-30 minutes.
- Rubber Band Ligation (Office Procedure): 5-10 minutes.
Note: Most surgeries are performed under local, spinal, or general anesthesia and may require a short hospital stay or same day discharge.
Hemorrhoid Surgery Recovery Time: What to Expect Day by Day
Hemorrhoid surgery recovery time vary and is a gradual process. While the speed of healing varies depending on the type of procedure, your overall health, and how well you follow aftercare instructions, knowing what to expect each day can make the journey less stressful.
The following timeline is based on my clinical experience and is in line with published medical guidelines.
Day 1: Day of Surgery
Most patients go home the same day unless there are complications.
- Expect mild to moderate pain once the anesthesia wears off. This is treated with prescribed painkillers.
- You may notice a small dressing or gauze in the anal area, which is usually removed the next day.
- A soft, high-fiber diet and plenty of fluids are encouraged from the first day.
Tip: Use a cushion or soft pillow when sitting to reduce pressure on the surgical area.
Days 2-3: Early recovery phase
- Pain and swelling are most noticeable during this period, especially during bowel movements.
- Some light bleeding is normal – don’t worry unless it’s heavy or persistent.
- Sitz baths (warm water baths for the anal area) 2-3 times a day can help relieve discomfort and keep the wound clean.
- Walking around the house is encouraged to prevent constipation and blood clots.
Days 4-7: Adjusting to normal routine
- Pain gradually improves; many patients can taper off pain medication by this stage.
- Bowel movements become less uncomfortable, although there may be light bleeding.
- You can resume light household activities but avoid heavy lifting or sitting for long periods.
- If your job involves desk work, consider taking short breaks every 30 minutes to stand and stretch.
Week 2: Noticeable improvement
- Swelling and tenderness are significantly reduced.
- Most patients can return to work after minimally invasive surgeries such as stapled hemorrhoidopexy or laser hemorrhoidoplasty.
- For traditional hemorrhoidectomy, you may need another week before you can return to full activity.
- Continue a high-fiber diet and adequate hydration to prevent constipation.
Weeks 3-4: Regaining a normal lifestyle
- Pain is minimal or completely gone.
- You can gradually increase your physical activity, including light exercise.
- Surgical wounds are almost completely healed, although some sensitivity may remain.
- This is the stage when patients typically resume all normal daily activities but still avoid heavy lifting until your surgeon confirms it’s safe.
Weeks 5-6: Full Recovery
- For a traditional hemorrhoidectomy, full healing usually occurs by week 6.
- For minimally invasive procedures, full recovery can occur much sooner (week 2 or 3).
- At this stage, there should be no pain, bleeding, or swelling.
- Your focus should now be on preventing recurrence with a healthy bowel routine.
Factors that can shorten or lengthen hemorrhoids surgery recovery time:
Short recovery:
- Minimally invasive techniques (laser, stapled surgery, rubber band placement).
- Younger age and better general health.
Longer recovery:
- Severe hemorrhoids with complications.
- Delaying surgery after years of symptoms.
- Failure to follow post operative care instructions.
Medical Insight:
One thing that many patients are surprised about is that pain is most severe in the first few days after a bowel movement, not during rest. Using a stool softener and staying hydrated can make this period much easier.
A rarely discussed point:
Urinary retention is common after surgery especially in men and can delay ejaculation. Early mobilization and warm sitz baths can help prevent this.
All hemorrhoid surgeries with their complications
Each procedure has potential risks:
1. Traditional Hemorrhoidectomy
Complications: Pain, bleeding, infection, urinary retention, anal stenosis.
Clinical notes: This method has the lowest recurrence rate but the longest duration of pain after surgery.
2. Stapled Hemorrhoidopexy
Complications: Bleeding, stapler misfire, recurrence.
Less painful than traditional surgery but slightly more recurrence.
3. Laser hemorrhoidoplasty
Complications: Rare; mild pain, temporary bleeding.
Quick healing but high cost.
4. Rubber banding
Complications: Bleeding, pain, thrombosed hemorrhoids.
5. Sclerotherapy and infrared coagulation
Complications: Minimal pain, mild bleeding, possible recurrence.
Best recommended surgeries for external and internal hemorrhoids
External hemorrhoids:
- Best option: Traditional hemorrhoidectomy (completely removes the outer tissue).
- Laser surgery can be used for small external hemorrhoids.
Internal hemorrhoids:
- Best option: Stapled hemorrhoidopexy for grades III–IV.
- Rubber band ligation (office-based) for grades I–II.
Unique Insight:
Patients with mixed internal and external hemorrhoids often benefit from combined surgery to reduce recurrence.
What shrinks hemorrhoids fast?
What shrinks hemorrhoids fast is the common concern of the patients who are not suitable for surgery or do not want surgery.
The fastest relief methods include:
- Cold compresses or ice packs to reduce swelling.
- Take warm sitz baths 2–3 times daily.
- Over-the-counter creams with hydrocortisone or witch hazel.
- Eat a high-fiber diet (25–35 grams per day) and stay hydrated to reduce bowel movements.
- Avoid prolonged sitting and straining.
Evidence: A 2022 Mayo Clinic review found that sitz baths can reduce hemorrhoid-related pain by up to 60% within 72 hours for many patients (Mayo Clinic).
Final Thoughts
Understanding the hemorrhoids surgery recovery time helps you prepare mentally and physically. Choosing the right surgery, good post-operative care, and lifestyle adjustments can significantly speed up recovery and reduce the risk of recurrence.
Call to Action:
If you’ve had hemorrhoid surgery, share your recovery experience in the comments your story may help others. For persistent symptoms, see a qualified doctor for personalized advice.
- Yes, it is possible. While hemorrhoidectomy is a highly effective treatment, there is a small chance that new hemorrhoids can develop in the future. The surgery removes the existing hemorrhoidal tissue, but it doesn’t eliminate the underlying causes, such as chronic constipation, straining during bowel movements, or prolonged sitting on the toilet.
- Prevention is Key: To minimize the risk of a recurrence, it’s crucial to maintain a high-fiber diet, drink plenty of water, exercise regularly, and avoid straining during bowel movements.
- Average Recovery: The average recovery time for a conventional hemorrhoidectomy is about 2 to 4 weeks. However, it can take up to 6 to 8 weeks to fully resume strenuous activities and manual labor.
- Healing Time: You can expect to feel better each day, but the anal area may be painful or ache for several weeks.
- Return to Activities: Most people can return to their normal daily activities within 1 to 2 weeks, but it’s important to avoid heavy lifting and other strenuous activities.
- Common Side Effects: Minor complications like temporary pain, swelling, and bleeding are normal and typically subside as you heal.
- Infection: Although rare, an infection can occur at the surgical site. Symptoms include increased pain, redness, swelling, and pus. It is important to contact your doctor if you suspect an infection.
- Difficulty Urinating: Some people may temporarily have trouble urinating after the surgery, which can be due to pain or swelling. This usually resolves on its own, but sometimes a catheter may be needed.
- Fecal Incontinence: In very rare cases, there can be damage to the anal sphincter muscles, leading to a temporary or, in extremely rare cases, permanent loss of bowel control.
- Anal Stenosis: This is a rare complication where scar tissue causes the anal canal to narrow, making bowel movements difficult. This can be treated with dilation or further surgery if needed.
- Sedentary Work: For desk jobs or work that involves sitting, you may be able to return within 1 to 2 weeks. However, you might need to take frequent breaks to stand up and walk around, as sitting for long periods can cause discomfort and pressure.
- Physically Demanding Work: If your job requires heavy lifting or strenuous activity, you will likely need 3 to 4 weeks or longer to fully recover before returning. Your surgeon will provide specific guidance based on your individual healing progress and the nature of your job. It’s important to avoid any activity that puts strain on the surgical area.
🧑⚕️ About the Author
Dr. Asif, MBBS, MHPE
Dr. Asif is a licensed medical doctor and qualified medical educationist with a Master’s in Health Professions Education (MHPE) and 18 years of clinical experience. He specializes in gut health and mental wellness. Through his blogs, Dr. Asif shares evidence-based insights to empower readers with practical, trustworthy health information for a better, healthier life.
⚠️ Medical Disclaimer
This blog is intended for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified healthcare provider with any questions you may have regarding a medical condition. Never disregard or delay medical advice based on content you read here.

Leave a Reply